Fact Checked
Intus Healthcare’s writers, customer service team, and sleep experts review and ensure this information is accurate.
Last updated on March 7th, 2024 at 10:16 am
COPD vs Asthma
Asthma and Chronic Obstructive Pulmonary Disease (COPD) are lung diseases that make breathing difficult. These conditions are often confused with each other. However, they affect the body differently and have distinct causes, symptoms, and management characteristics. This article will explain the similarities and differences between the conditions.
Table of Contents
What is COPD?
Chronic Obstructive Pulmonary Disease is the collective term for several lung diseases that prevent proper breathing. Two of the most common COPD conditions are emphysema and chronic bronchitis. These conditions can occur separately or together.
What is Asthma?
Asthma is a lung condition that causes the airways to narrow, making breathing difficult. It is typically less progressive than COPD.
The overlap between Asthma and COPD
Asthma and COPD share similar symptoms, which can lead to misdiagnosis and delayed treatment. Common symptoms include wheezing, coughing, shortness of breath, and chest tightness, which can vary in severity and frequency.
Causes
COPD: Typically, COPD is caused by long-term exposure to harmful substances, primarily cigarette smoke, as well as environmental pollutants, occupational dust, or chemical fumes. Smoking is the leading cause of the disease; a study found 50% of smokers eventually develop COPD (1). This is because the smoke irritates the lungs, reducing the natural elasticity of the bronchial tubes and air sacs, leading to over-expansion and trapped air in the lungs during exhalation.
Genetic factors can also play a role. Around 1% of sufferers develop the condition due to a rare genetic disorder that reduces the level of the protein alpha-1-antitrypsin (AAT). However, many people with AAT deficiency do not have symptoms, or if they do, these symptoms only arise between the ages of 20 and 50.
Asthma: It is not clearly understood why some people develop asthma. It is often associated with allergies and is therefore considered an allergic disease. It is commonly caused by a hyperreactive immune response to various triggers like allergens, respiratory infections, pollen, mould, pet hair, exercise, smoke, stress, or cold air. Genetics play a more significant role in asthma susceptibility, but this differs from person to person.
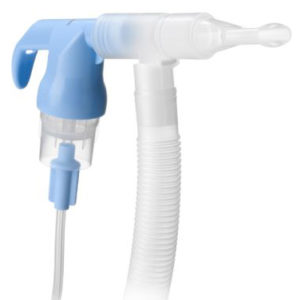
Nebulisers
We offer a variety of daily-use Microlife nebulisers to treat Asthma, COPD and other respiratory conditions. The small devices deliver medication in a mist through a mouthpiece to ease symptoms and provide fast relief. Explore our mains-powered and portable nebuliser machines below.
The effect the conditions have on lung function
COPD: The lung function of individuals with COPD is characterised by a persistent decrease in airflow due to narrowed airways. This leads to a diminished forced expiratory volume (FEV1) compared to normal, indicating a reduced airflow. In COPD, there is chronic inflammation of the airways, which produces excessive mucus and narrowing of the bronchial tubes (airways). This inflammation makes it difficult for air to move in and out of the lungs efficiently. As COPD advances, the impaired gas exchange in the lungs can lead to lower oxygen levels (hypoxia) and higher blood carbon dioxide levels (hypercapnia). This can result in symptoms like shortness of breath, cyanosis (bluish discolouration of the skin and lips) and altered mental status. The effects of COPD on the lungs are irreversible but can be managed with the correct treatment.
Asthma: The condition causes airway inflammation, muscle tightness and excess mucus production. During asthma exacerbations or attacks, lung function can significantly decrease. During an asthma attack, forced expiratory volume (FEV1) decreases due to airway obstruction. However, with appropriate treatment, lung function can improve, and FEV1 can return to normal or near-normal levels.
The influence of age
COPD: The disease usually develops later in life, often after years of exposure to risk factors like smoking or occupational hazards. It is most common in individuals over the age of 40.
Asthma: Asthma can develop at any age, including childhood. It often presents in childhood and may persist into adulthood, but it can also develop in adults with no prior history of asthma.
Reversibility
One of the key distinctions is that COPD is typically not reversible. The airway damage caused by COPD is usually permanent, and treatment focuses on symptom management and slowing disease progression.
On the other hand, asthma symptoms are often reversible, especially in response to bronchodilator medications (such as inhalers containing Albuterol) or anti-inflammatory drugs (like corticosteroids). Asthma symptoms can improve with proper management, and many asthma patients lead relatively normal everyday lives with effective treatment.

Diagnosis
If you have consistent symptoms of either disease, you should visit your healthcare provider to determine if you have one of the conditions.
COPD: To help diagnose the disease, your GP may ask specific questions and examine you; these may include:
- A chest examination to listen to your breathing.
- Ask about your symptoms.
- Ask if you smoke.
- Calculate your BMI.
- Ask about your family history in terms of lung conditions and problems.
You may also be required to complete various lung function tests. Typically, patients must complete a spirometry breathing test to show how well their lungs are working.
When completing a spirometry test, you will be required to blow forcefully into a spirometry machine. The machine measures the volume of air you can exhale in one second and the total volume of air you breathe out. Your results are compared to expected results for someone of your age.
Chest X-rays and blood tests may also be used to test for COPD.
Asthma: Your GP may ask specific questions to help the diagnosis; these may include:
- Details about your symptoms
- If anything triggers asthma attacks
- If you have eczema, allergies, or a family history of them.
You may also be required to complete some tests to help confirm the condition. The main tests used to diagnose asthma include:
- FeNO – This test requires you to breathe into the device to measure the nitric oxide level in your breath.
- Peak flow test – This requires you to breathe into a handheld device to measure how fast you breathe out.
- Spirometry testing with reversibility – The device requires you to blow forcefully to measure how fast you can breathe out and how much air you can hold. Depending on the result of your spirometry, you may be given an inhaler and then asked to repeat the spirometry test to see if there has been a significant improvement.
Treatment
COPD: Treatment for COPD typically involves:
- Bronchodilator inhalers, steroid inhalers, or nebulisers to deliver medicine directly to the lungs to make breathing easier.
- Theophylline tablets, Mucolytics, Steroid tablets, or antibiotics
- Lifestyle adjustments such as quitting smoking and engaging in regular exercise to improve muscle strength.
Asthma: Asthma management includes:
- Various inhalers: Bronchodilators, steroid inhalers, reliever inhalers, preventer inhalers and combination inhalers to deliver medication.
- Theophylline or steroid tablets.
- Nasal irrigation can also help to manage symptoms.
For some individuals with severe asthma, these treatments do not help, and they are recommended biologic therapy injections or bronchial thermoplasty surgery.

Comorbidities
Comorbidities are conditions that you can have alongside the primary disease. Research found that more than 20% of COPD sufferers have three or more comorbid conditions (2).
The comorbidities of asthma and COPD are often similar; these include:
- Cancer
- Stomach ulcers
- Sinusitis
- High blood pressure
- Sleep disorders – Insomnia and Obstructive Sleep Apnoea (OSA)
- Depression and anxiety
- Diabetes
- Gastro-Oesophageal Reflux Disease (GERD)
- Cardiovascular conditions
- Chronic infections
Summary
In summary, while both COPD and asthma share similarities in symptoms and airway inflammation, they have different underlying causes, age of onset, reversibility of airflow obstruction, and treatment approaches. Accurate diagnosis and appropriate management are crucial to provide the best care for individuals with these conditions. If you or someone you know is experiencing respiratory symptoms, it’s essential to consult a healthcare professional for a thorough evaluation and diagnosis.
If you think your breathing condition could be related to OSA, please see our Sleep Apnoea Symptoms page. If you have symptoms of the sleep condition, you can take our free online Sleep Apnoea Risk Test to determine if you could have OSA.
REFERENCES
- Lundback B, Lindberg A, Lindstrom M, Rönmark E, Jonsson AC, Jönsson E, Larsson LG, Andersson S, Sandström T, Larsson K. Not 15 but 50% of smokers develop COPD? Report from the Obstructive Lung Disease in Northern Sweden Studies. Respir. Med. 2003;97:115–122. Available at: https://pubmed.ncbi.nlm.nih.gov/12587960/. Accessed: 30.01.24
- Van Manen JG, Bindels PJ, IJzermans CJ, van der Zee JS, Bottema BJ, Schadé E. Prevalence of comorbidity in patients with a chronic airway obstruction and controls over the age of 40. J Clin Epidemiol. 2001 Mar;54(3):287-93. doi: 10.1016/s0895-4356(01)00346-8. PMID: 11223326. Available at: https://pubmed.ncbi.nlm.nih.gov/11223326/. Accessed: 30.01.24