Fact Checked
Intus Healthcare’s writers, customer service team, and sleep experts review and ensure this information is accurate.
Last updated on February 16th, 2024 at 03:25 pm
Want to identify if your husband, wife or partner has Sleep Apnoea?
If you have arrived at this page, you have likely identified some potential warning signs that your husband, wife or partner may have Sleep Apnoea. If you are losing sleep because of your bed partner’s snoring or you have noticed pauses in their breathing, this article will help you understand the symptoms, explain more about the condition, the dangers and how you can find out if Sleep Apnoea is the cause of their sleep problems.
What is Sleep Apnoea?
Sleep Apnoea is a sleep disorder that is characterized by pauses in breathing or shallow breathing during sleep. These pauses in breathing, called Apnoea’s, can last up to several minutes and occur multiple times an hour. As a result, people with Sleep Apnoea often wake up feeling tired or unrefreshed, even if they have slept for a full night.
There are three main types of Sleep Apnoea:
- Obstructive Sleep Apnoea (OSA): This is the most common type of Sleep Apnoea and occurs when the muscles in the back of the throat fail to keep the airway open, leading to complete blockages.
- Central Sleep Apnoea: This type of Sleep Apnoea occurs when the brain fails to send the proper signals to the muscles that control breathing.
- Complex Sleep Apnoea syndrome (formerly known as mixed Sleep Apnoea): This type of Sleep Apnoea is a combination of both obstructive and central Sleep Apnoea.
There are different severities of Sleep Apnoea: mild, moderate, and severe. OSA severity is calculated by the apnoea-hypopnea index (AHI), which indicates how many breathing pauses happen per hour each night. The British Lung Foundation found up to 85% of people with OSA are undiagnosed and untreated(1).
Sleep Apnoea Warning Signs
There are different symptoms and warning signs that could indicate that your partner may have Sleep Apnoea. These include:
- Snoring – A primary warning sign of Sleep Apnoea is snoring. Snoring occurs when the muscles in the throat relax during sleep, causing the airway to narrow or become partially blocked. This can cause the air moving through the airway to vibrate the surrounding tissues, leading to the sound of snoring. Not everyone who snores has Sleep Apnoea, but snoring can be a sign of a potential problem with sleep-related breathing.
- Choking during sleep – Choking and gasping for air at night is a strong indicator of OSA. The airway blockages cause people to stop breathing for a moment, resulting in waking up choking.
- Daytime sleepiness – People with Sleep Apnoea often experience daytime sleepiness because their sleep is disrupted by pauses in breathing or shallow breathing during sleep. This can lead to a lack of deep, restorative sleep, which can make it difficult to stay awake and alert during the day
- Brain fog – When we sleep, our bodies go through a REM cycle; when Sleep Apnoea interrupts this, it causes a chemical imbalance which impacts the brain, causing insufficient concentration, memory loss and brain fog.
- Morning headaches – Headaches upon waking in the morning are a common complaint among people with Sleep Apnoea. These headaches can be caused by repeated episodes of partial or complete blockage of the airway during sleep, which can lead to a lack of oxygen in the brain. This lack of oxygen can cause inflammation and swelling in the blood vessels in the brain, leading to headaches.
- Waking with a dry mouth – A dry mouth in the morning results from repeated episodes of partial or complete blockage of the airway during sleep. This leads to reduced airflow and a decrease in saliva production. This decrease in saliva can cause the mouth to feel dry and uncomfortable.
- Nocturia – People do not usually connect this to Sleep Apnoea, but Nocturia is when someone wakes up too frequently during the night to urinate. Repeated episodes of partial or complete blockage of the airway during sleep, can lead to an increase in blood pressure and a strain on the kidneys. This can cause the kidneys to produce more urine and an increased need to urinate at night.
- Mood – Mood changes, including irritability and difficulty with mood regulation, are common among people with Sleep Apnoea. This can be caused by disrupted sleep and a lack of deep, restorative sleep. Poor sleep quality can lead to a decrease in the production of neurotransmitters, such as serotonin and dopamine, which play a role in mood regulation.
You can also take a look at the Epworth Sleepiness Scale; the questionnaire lets you know the risk of having Sleep Apnoea.
Sleep Apnoea symptoms in men and women are the same, and it is estimated that 20% of women have moderate Sleep Apnoea(2). We have a dedicated page which talks in detail about the Symptoms of Sleep Apnoea.

What does Sleep Apnoea sound like?
Most people discover they have OSA because someone else has heard how they breathe during sleep. If you want to listen to an example of someone with Sleep Apnoea, here is what Sleep Apnoea sounds like.
People who struggle with OSA have laboured breathing, including snoring, gasping, choking, and snorting, all caused by the strain on their airways. Sleep Apnoea can be loud; you may also find your partner has deep, shallow breaths and periods of silence. In cases of severe Sleep Apnoea, people can stop breathing over 30 times an hour per night.
The dangers of OSA
Untreated Obstructive Sleep Apnoea can severely impact your and your partner’s quality of life, and untreated OSA can have serious consequences, including:
– Increased risk of high blood pressure: OSA can cause an increase in blood pressure, which can increase the risk of heart attack and stroke.
– Cardiovascular problems: OSA has been linked to an increased risk of heart attack, stroke and other cardiovascular problems.
– Memory and concentration problems: The lack of oxygen that occurs during episodes of OSA can cause problems with memory and concentration.
– Mood changes and irritability: OSA can cause mood changes and irritability because of the disrupted sleep and lack of deep, restorative sleep that often occurs in people with the disorder.
If your partner, husband, or wife is experiencing symptoms of OSA, it is important to speak to a healthcare provider. They can help to diagnose the cause of your symptoms and recommend appropriate treatment, which may include lifestyle changes, such as losing weight and quitting smoking, and the use of treatment, such as Continuous Positive Airway Pressure (CPAP) machines, which can help to keep the airway open during sleep. Treatment can help to reduce the risk of the serious consequences of OSA and improve your overall health and well-being.
What to do if your partner has Sleep Apnoea
Seek treatment. Sleep Apnoea can’t be cured, but the symptoms can be treated and reduced. The severity of someone’s OSA will influence the required treatment, but possible treatments include:
- Continuous Positive Airway Pressure (CPAP) – CPAP therapy is the most popular Sleep Apnoea treatment widely used. A CPAP device provides air pressure through a CPAP mask to keep the airway open. The positive air pressure stops the airway from closing and collapsing, which prevents the pauses in breathing (Apnoea’s).
- Mandibular Advancement Device (MAD) – Suitable for those with mild or moderate Sleep Apnoea. A Mandibular Advancement Device is a good alternative to CPAP therapy. It is a mouth guard device that pulls your lower jaw and tongue forward, creating more space at the back of the throat, reducing and sometimes preventing Apnoeas and snoring.
- Somnibel Positional Sleep Therapy Trainer – This device is for those with positional Sleep Apnoea. The Positional Therapy Trainer sits on the forehead and vibrates when the user turns during the night to sleep on their back. The vibration would encourage them to turn back onto their side. Side sleeping is a recommended position to stop or reduce Apnoeas.
Can I test myself for Sleep Apnoea?
If you think you could have Sleep Apnoea, why not take a sleep test?
If you need further information, please do not hesitate to contact us.
Identifying Sleep Apnoea: Take an In-Home Sleep Test
If your partner is experiencing some or all these symptoms, they could have Sleep Apnoea. You should contact your GP, and a referral may be made to a sleep clinic to be tested. The waiting list for a sleep study on the NHS can be as long as two years, so if you need a result faster, you may wish to do a confidential and accurate In-Home Sleep Test instead.
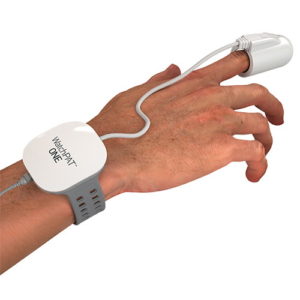
Our home sleep test device will monitor the same parameters as a sleep clinic study. It will measure snoring intensity, blood oxygen levels, body position, heart rate, body movements, and Peripheral Arterial Tone (PAT).
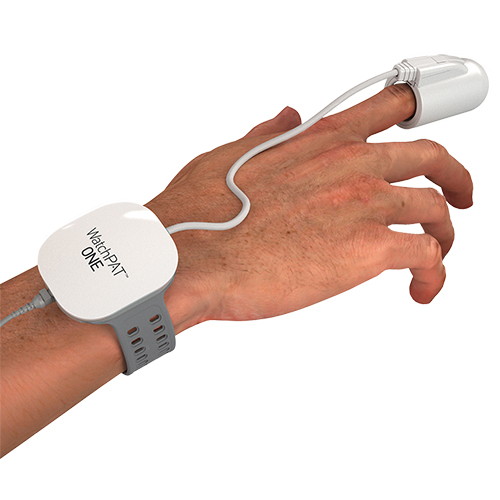
The device is worn for one night at home and once completed, our experienced NHS trained sleep technicians will analyse the data. A detailed sleep report is produced based on the results, confirming if you have OSA or not.
The results of your sleep test will only be sent to you. We do not send your results to the DVLA or your GP. It is up to you to take the next step.
The sleep test can also rule out Sleep Apnoea, enabling you to focus on other things that could be causing the sleep problems.
REFERENCES
- BLF (2015) Obstructive sleep apnoea (OSA) – asthma + lung UK, Obstructive Sleep Apnoea (OSA). Available at: https://www.blf.org.uk/sites/default/files/OSA_Toolkit_2015_BLF_0.pdf. Accessed: 09.08.23.
- Franklin, K.A. et al. (2012) ‘Sleep Apnoea is a common occurrence in females’, European Respiratory Journal, 41(3), pp. 610–615. doi:10.1183/09031936.00212711. Accessed: 09.08.23.